Osteoarthritis (OA) is the breaking down of cartilage over time. Most people assume to comes along with getting older. This is partially true, however there is much more to it than that. As our global population ages, it is projected that by the year 2030, 25% of the adult population will be affected by osteoarthritis.(1) This condition alone cost the health care system 300 billion dollars annually.(1) As knee OA, gets worse it can often lead to pain, impaired quadriceps muscle strength, decreased range of motion, and functional limitations.(1) Over time, increased pain levels and decreased function affect patients’ motivation and willingness to move or participate in an exercise program.(1)
The use of sEMG biofeedback can prove imperative for helping address the effects of knee osteoarthritis. Before we look at how mTrigger biofeedback can be used to help patients struggling with knee OA, its important to first understand what the literature says is happening at a physiological level.
The Science
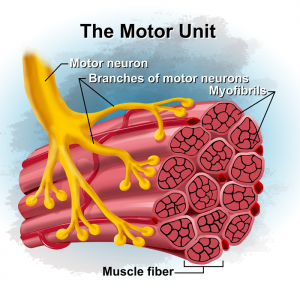
Surface EMG measures the electrical activity of the contracting motor unit of skeletal muscle (in this case the quadriceps). Each motor unit consists of a single lower motor neuron and all the muscle fibers it innervates (see image).(2) As the quad muscle contracts, the number and size of the firing motor units is going to be directly related to the force of the muscle contraction.(2) Once a motor unit fires, all fibers in that motor unit will contract simultaneously.(2) The Henneman’s size principle tells us that smaller motor units will be activated first, followed by progressively larger ones as force demands increase.(2) This seems simple enough; as muscle demands increase, more (and larger) motor units are called upon to meet the demand of the task. While this is true, as individuals get older, age-related changes occur in the muscle.(2) Neurological alterations, changes in the motor neuron, motor unit, and muscle compensation all effect the quadriceps muscle and its role in osteoarthritis.(2)
The Studies
EMG data in patients with knee OA demonstrates age related changes in quadricep motor unit recruitment patterns during progressively more difficult tasks.(2) In one study, participants with varying severities of osteoarthritis were compared to a control group during different functional tasks.(2) What researchers found is interesting. Quad muscle activation strategies varied significantly between patients with osteoarthritis and the control group as well as between patients with different severities of OA.(2) As a whole, the amount of strength loss observed was correlated to the severity of knee OA. (2) Furthermore, sEMG amplitude of the quad during functional exercise was much lower in more severe cases.(2) This means that as a higher effort contraction was required, there was an even smaller relative increase in the amplitude of the muscle contraction.(2) Typically, we expect to see an equivalent increase in EMG amplitude of the quad muscle as the contraction demand increases. Patients with more severe OA, achieved the desired force by activating more and larger motor units per unit of force, even during lower magnitude tasks.(2) In less severe cases, patients activated larger but fewer motor units.(2) All this to say, knee osteoarthritis appears to alter the normal motor unit firing pattern observed in skeletal muscle. This faulty firing pattern led to a reduced force accuracy (tendency to overshoot) and less steadiness during functional exercise.(2)
A large factor in the firing pattern displayed by patients with varying levels of osteoarthritis has to do with inactivity and immobilization.(2) In a muscle that is not used, immobilized, or injured, the un-used motor fibers begin to re-organize into larger motor units as they are adopted by adjacent lower motor neurons.(2) Now, to achieve a task, motor units are firing simultaneously (all at the same time) instead of by Henneman’s size principle.(2)
Clinical Application
In these studies, sEMG biofeedback was used to help understand what was occurring in the quad muscle in patients with knee osteoarthritis. Now, lets look at how mTrigger biofeedback be used to help improve the health, mobility, and functional loss that coincides with knee OA.
It is recommended patients with knee OA perform an exercise program derived by a physical therapist 2-3x a week focused on strengthening, education, and remaining active.(3) However, adherence to these programs is very low with a large group of patients not responding favorably.(3)
As noted earlier, patients with knee OA tend to inefficiently activate their muscles (seen as an increase in amplitude, larger motor units, and prolonged duration of contraction).(2,3) This lack of strength can lead to an increase in mechanical stress on the articular cartilage, bone, joint capsule, and surrounding soft tissues of the knee joint.(3) As a result, nociceptive input and pain levels often increase as well.(3) The goal clinically is to help increase the EMG activity of the quadriceps muscle during functional exercises. Over time this helps to improve the motor unit recruitment pattern and increase cortical activity thereby improving strength. Furthermore, this increase in strength can also help to provide a cushioning effect to the joint for better shock absorption.
To help address these issues, mTrigger sEMG biofeedback can be used to teach patients how to perform functional movements and exercise by properly activating the quad muscles.(3) By working through functional tasks such as a step up or squat with mTrigger biofeedback, patients are able to problem solve through obtaining proper movement with the goal of increasing overall sEMG activity and muscle activation.
Additionally, during mid stance of gait, faulty quad activation is also commonly observed with knee OA. mTrigger biofeedback along with therapist cueing can be a way to help improve motor patterns and promote learning.(3)
The implementation of biofeedback during functional tasks was shown to help improve patients’ willingness to work through functional exercises they may have previously avoided due to discomfort.(3) These patients felt that biofeedback provided them with the opportunity to change the way they moved giving them more control over their pain, symptoms, and treatment.(3)
In addition, patients with knee OA develop compensatory movement patterns that persist, even after a joint replacement is performed.(4) Compensations such as off-loading the involved side, asymmetries between limbs, quad weakness, and poor physical function are just a few examples.(4) Biofeedback was used in this particular study to help decrease compensatory movements that increase load and potential development of OA on the contralateral side, by working to improve weight bearing activities (such as a squat), movement patterns, strength, and patient engagement in exercise following surgery.(4)
Numerous studies have demonstrated quad weakness as a result of avoidance of activity and a common symptom of OA.(3) In this populations especially, the need for increasing sEMG output and thereby strength is imperative for long term success.
Summary
mTrigger biofeedback is an excellent tool to help patients with all severities of knee OA learn to perform functional exercises with less pain and better technique. By receiving biofeedback on muscle activation and movement compensations patterns, patients are given the opportunity to change the way they move allowing them to feel more control over their pain, symptoms, and treatment.(3) Implementing mTrigger biofeedback for knee OA rehabilitation programs can help to improve muscle activation, compliance, engagement, and overall satisfaction throughout the rehab process.
References
1. Krepkovich E, Kaur M, Mangum LC, et al. Feasibility of a Novel Video Game-Based Electromyography Biofeedback System in Patients With Knee Osteoarthritis. J Sport Rehabil. 2022;31(7):937. doi:10.1123/JSR.2021-0397
2. Ling SM, Conwit RA, Talbot L, et al. Electromyographic patterns suggest changes in motor unit physiology associated with early osteoarthritis of the knee. Osteoarthritis Cartilage. 2007;15(10):1134-1140. doi:10.1016/J.JOCA.2007.03.024
3. Preece SJ, Brookes N, Williams AE, et al. A new integrated behavioural intervention for knee osteoarthritis: development and pilot study. BMC Musculoskelet Disord. 2021;22(1). doi:10.1186/S12891-021-04389-0
4. Bade MJ, Christensen JC, Zeni JA, et al. Movement Pattern Biofeedback Training after Total Knee Arthroplasty: Randomized Clinical Trial Protocol. Contemp Clin Trials. 2020;91:105973. doi:10.1016/J.CCT.2020.105973
Image: https://chadwaterbury.com/the-science-of-motor-unit-recruitment-part-1/
mTrigger Biofeedback for Older Adults
|
Promoting Motor Learning with Biofeedback
|








Leave A Comment