with Mark Callanen, PT, DPT, OCS | Director of Clinical Development, LightForce® Therapy Lasers
Originally featured on LightForceMedical.com
Being an orthopedic physical therapist for over 20 years allows you to see a lot of post-operative knees. While in practice I tried to balance evidence-based approaches with acquired clinical knowledge to generate successful outcomes on a regular basis. Most would agree, this usually requires a combination of appropriate manual techniques, exercise-based treatments, a touch of psychology, and the use of a few choice modalities along the way.
Background and Procedure
Recently I had a unique opportunity to experience the rehabilitation process from a patient’s perspective after having 50% of my right medial meniscus removed. I had been having significant clicking and medial joint line pain for 6 months prior to surgery. No spectacular episode to reflect back on other than years of wear and tear.
Prior to surgery my knee was progressively worsening. The primary complaint was notable clicking as the knee approached terminal extension during hill walking and light treadmill jogging. Deep knee flexion was also uncomfortable and any quick lateral motion was not well tolerated. Once I accepted the fact that my almost 50-year-old cartilage needed some surgical help, I scheduled the orthopedic consult.
After surgery, I decided I would play the part of both patient and therapist during my rehab. I was curious to see if my personal concepts regarding the management of acute inflammation would hold up. The surgery was scheduled on a Friday morning and I was home by lunch time. A text book posterior horn medial meniscectomy was performed without complication. The only other tissue that was addressed during the arthroscopy was the removal of thickened plica from my medial joint capsule. The knee was flushed with anesthetic (20 cc of 0.5% ropivacaine) after the procedure to help control pain.
Post-Op
Post-operative instructions were to keep the dressing in place for 5 days with instructions to keep the bandage dry while icing and elevating the knee as needed for up to 2 weeks. Instruction was also given to take 800 mg ibuprofen every 4-6 hours during that time and take opioids (Norco) for pain as needed. Regarding rehab, instructions were to start bending knee as tolerated and begin rehab at an out-patient PT facility the following week.
Pretty standard instructions that most clinicians could predict in their sleep. I of course did almost NONE of these things. I removed the outer dressing within 2 hours of getting home to expose the skin and allow me to inspect the swelling. I covered the portal sites with band aids to prevent infection. Removing the bandages made it easier to bend the knee and range the joint. Exposing the skin also enabled laser treatments to begin on day one.
4-5 hours post-surgery, I had minimal pain due to the anesthetic that was injected in the knee. I wanted to take advantage of this time period with reduced pain to see how the knee was moving and if the quad was firing. To my surprise, I had about 80% of knee flexion ROM and the quad was still able to volitionally contract.
Since I had quadriceps control, I was able to walk and bear weight almost immediately without significant pain or difficulty. I did not require an assistive device. My primary goals were to reduce swelling quickly in order to maintain volitional VMO control, and restore normal ROM as quickly as possible to avoid stiffness/ scar formation in the capsule.
So what tools did I plan to use to help accomplish these goals?
Fortunately, as the Director of Clinical Development at LightForce, I have access to a Class 4 laser and other devices that enabled me to quickly progress my program. In addition to the laser, I was also able to utilize 2 other modalities to assist during my recovery; an mTrigger biofeedback unit as well as a negative pressure device (LymphaTouch) designed to help with swelling and scar tissue mobility.
Given the current research on cryotherapy (1), I was not planning to utilize ice unless there was a significant amount of joint effusion. Luckily, that wasn’t the case. I focused on pursuing active healing in order to promote better blood flow and try to abate the inflammatory cascade.
Photobiomodulation via LightForce Class 4 Laser Therapy
4 hours after surgery I began lasering my knee to promote photobiomodulation. Treatment areas included all exposed areas of the joint and the distal quadriceps except for the incision sites. Treatment was performed in a circumferential fashion. Settings were in the 6-8 J/cm2 range for the first week. Power ranged from 6 Watts to start and progressed by 2 Watts a day for the first two weeks. I capped power at 25 Watts. Treatment was performed 2 x day for the first 5 days, and every other day the second week due to the progress that was observed.
Swelling improved each day due to the effects of photobiomodulation and volitional quadriceps activities. Open and closed chain strengthening started 2 days after surgery at a local gym. ROM was restored to WNL within 3 days after the surgery with pain never going above 3/10 at any point in the process. NSAIDS were discontinued after 2 days and the opioid prescription was never filled.
Neuromuscular Assessment via mTrigger Biofeedback
I received the mTrigger a couple days after the surgery date. It quickly pointed out that my EMG activity was at about 50% of my non-involved quad when training it with quad sets and straight leg raises. This was not surprising, but at 2 weeks after surgery, where I had been doing unilateral leg extension exercises in a gym with 20-30 lbs, I was amazed to see that motor firing was still operating at a 20% deficit! I would have had no way to appreciate this without the mTrigger device.
A 2010 study confirmed that EMG activity is often decreased at 6 months after medial meniscectomy surgery. This deficit is present in cases where there is no difference in muscle control at submaximal levels and there is equivalent muscle architecture to the uninvolved side. The study concluded the deficit is likely attributable to neural impairments that affect muscle control at maximal force outputs (2).
The study confirmed what I experienced. Even with minimal swelling at the knee, no significant pain, and a volitional muscle contraction in place while under a submaximal load, my medial quadriceps was not firing normally. It highlighted that retraining quadriceps activity after surgery is a longer process than I had previously appreciated. Not doing so increases the chance of reinjury for weekend warriors that return to sport with the quad in this state. Using tools like NMES and biofeedback should help address this problem.
Lymph Management via Negative Pressure LymphaTouch
The last modality I was able to introduce to my program was a negative pressure LymphaTouch device. I was not able to apply it to my knee during my first week of rehab due to logistical reasons, which was unfortunate as it would have been great in helping with lymph flow around the knee.
Since there was plica removed from my medial capsule, there was more swelling at the medial capsule than other parts of the knee. There were a handful of other areas that stood out as being sore with palpation: namely the bursa directly over the patella, the fibular head, and the lateral joint line proximal to the fibular head.
Applying the LymphaTouch device with moderate suction, 125-175 mm Hg in an intermittent setting, helped with reducing residual swelling around the medial knee and patellar area during the 4 weeks after surgery. Using the device in a constant setting with higher suction (250 mm HG) allowed for myofascial treatments over areas that were more tender. The pulling and twisting of the tissue helped with soreness in the soft tissues that were difficult to address otherwise. Self-massage did not seem to impact it effectively.
Treatment with the LymphaTouch was performed over the problem areas 3-4 times a week. This helped minimize soft tissue complaints by the end of week 4, where I was able to start kneeling on the knee with minimal pain. Once the incisions were completely closed at 3 weeks, the negative pressure treatments also helped reduce pain and swelling around the portal sites. Currently there is no abnormal tissue texture noted over the portal sites or any other area of the knee.
Exercise
Regarding exercise, a progressive lower extremity strength, balance, and ROM program started the day after surgery at a local gym. Activities on the day of surgery focused on heel slides, quad sets, and restoring normal gait mechanics. Starting on day 2, leg exercises were performed 3 x week in some variation of closed/ open chain activity with a treadmill progression to return to jogging. Closed chain exercises were able to be introduced 2 days after surgery due to lack of pain and swelling.
What did this active approach to knee rehab accomplish?
- Weight bearing started within hours of surgery. Over 90% of ROM was restored in 2 days and full ROM in 4 days. Volitional VMO control was never lost enabling hip and quad exercises to begin in the gym 2 days after surgery.
- Jogging in small one-minute bouts began in the second week. Prior to surgery I was unable to jog on a treadmill without pain/ clicking. NSAIDS were used for 2 days after surgery, but all medicines were discontinued 3 days after surgery without ever having pain over 3/10 level.
- Surgery was performed on a Friday and I was able to walk up to a second story the following Tuesday and sit comfortably at my desk for 6 hours.
Closing Thoughts
A couple closing notes. My surgery was performed by an experienced orthopedic physician. His ability to perform the procedure without unwanted disruption in other areas of the knee was evident by the lack of swelling after the treatment. A quick recovery is often dependent on a successful surgery.
Another component that may have impacted post-operative swelling was a phenomenon referred to as preconditioning (3). My knee was treated with high power laser 2-3 x week for several months prior to surgery in order to control swelling and pain. I walked into surgery without a pain complaint.
Preconditioning has been shown to help reduce inflammatory responses by preventing apoptosis when cells are placed under oxidative stress. It may have been another component as to why I experienced limited swelling after the surgery.
In a perfect world I would have started the negative pressure treatments on day one to assist the lymph system, but introducing this technology a week after surgery did not seem to negatively impact my progress. Starting the assault on the inflammatory cascade early on with the laser seemed to play a huge part in my painless progression into moderate level activity in less than a week.
Rehabilitation specialists should also be acutely aware of the neural deficits that may be lingering during and after the subacute stage of recovery. Progressing patients to higher level activities based solely on observational findings could prove to be detrimental to the knee if muscle function is not assessed with some form of biofeedback.
Finally, for those clinicians that are still heavily invested in cold modalities; it is worth reiterating that going with an active rehabilitation program is what drove this success story. Cryotherapy was not used at any point following surgery to address pain or inflammation.
References
- Reinl G. ICED! The Illusionary Treatment Option. Oct 15, 2013: 9-11.
- Glatthorn JF, Berendts AM, Bizzini M, Munzinger U, Maffiuletti NA. Neuromuscular function after arthroscopic partial meniscectomy. Clin Orthop Relat Res. 2010;468(5):1336-1343. doi:10.1007/s11999-009-1172-4
- Agrawal T, Gupta GK, Rai V, Carroll JD, Hamblin MR. Pre-Conditioning with Low-Level Laser (Light) Therapy: Light before the Storm. Dose-Response. October 2014.
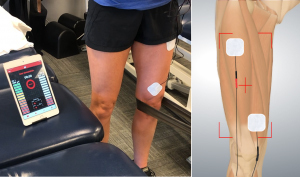
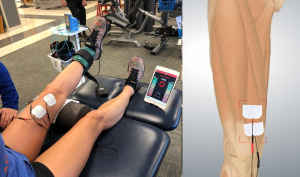
Best Practices for Placement
-
For example, if you want a picture of activity across the whole quad, try a placement like this Isolated placement: The photo on the left shows two channels of input monitoring the medial and lateral quads; the diagram on the right shows isolated monitoring of the VMO.
[closing]
For more on best practices:
Visit Setup & Training Page BUY ELECTRODES Let us know what you’d like to see more of on our blog by commenting below or getting in touch.






Leave A Comment